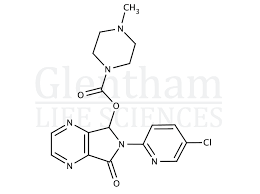
Buy Zopiclone (Imovane) Cas 43200-80-2
Zopiclone, sold under the brand name Imovane among others, is a nonbenzodiazepine, specifically a cyclopyrrolone, used to treat insomnia. While molecularly distinct from benzodiazepine drugs, Zopiclone’s mechanism of action is similar; it increases the normal transmission of the neurotransmitter gamma-aminobutyric acid (GABA) in the central nervous system, via positive allosteric modulation at GABAA neurons.
Zopiclone is considered a sedative and CNS depressant. After prolonged use, the body can become accustomed to the effects of zopiclone. When the dose is then reduced or the drug is abruptly stopped, withdrawal symptoms may result. These can include a range of symptoms similar to those of benzodiazepine withdrawal. Although withdrawal symptoms from therapeutic doses of zopiclone and its isomers (i.e., eszopiclone) do not typically present with convulsions and are therefore not considered life-threatening, patients may experience such significant agitation or anxiety that they seek emergency medical attention. [citation needed]
In the United States, zopiclone is not commercially available,[4] although its active stereoisomer, eszopiclone, is. Zopiclone is a controlled substance in the United States, Japan, Brazil, New Zealand and some European countries, and may be illegal to possess without a prescription. [citation needed]
Zopiclone is known colloquially as a “Z-drug“. Other Z-drugs include zaleplon and zolpidem and were initially thought to be less addictive than benzodiazepines. However, this appraisal has shifted somewhat in the last few years as cases of addiction and habituation have been presented. Zopiclone is recommended to be taken at the lowest effective dose, with a duration of 2–3 weeks for short-term insomnia.[5] Daily or continuous use of the drug is not usually advised, and caution must be taken when the compound is used in conjunction with benzodiazepines, sedatives or other drugs affecting the central nervous system.[6]
Medical uses

Zopiclone is used for the short-term treatment of insomnia where difficulty with sleep initiation or sleep maintenance are prominent symptoms. Long-term use is not recommended, as tolerance, dependence, and addiction can occur.[7][8] One low-quality study found that zopiclone is ineffective in improving sleep quality or increasing sleep time in shift workers, and more research in this area has been recommended.[9]
Cognitive behavioral therapy has been found to be superior to zopiclone in the treatment of insomnia and has been found to have lasting effects on sleep quality for at least a year after therapy.[10][11][12][13]
Long-term use of Z-drugs, including zopiclone, has been associated with dependence, withdrawal symptoms, and cognitive impairment.[14]
Alternative approaches such as lifestyle modification, melatonin supplementation, mindfulness, and certain traditional herbal medicines (e.g., Ashwagandha, Brahmi, Jatamansi) have been explored as supportive options for managing insomnia, though further clinical research is required.
Specific populations
Elderly
Zopiclone, similar to other benzodiazepines and nonbenzodiazepine hypnotic drugs, causes impairments in body balance and standing steadiness in individuals who wake up at night or the next morning. Falls and hip fractures are frequently reported. The combination with alcohol consumption increases these impairments. Partial, but incomplete tolerance develops to these impairments.[15] Zopiclone increases postural sway and increases the number of falls in older people, as well as cognitive side effects. Falls are a significant cause of death in older people.[16][17][18]
An extensive review of the medical literature regarding the management of insomnia and the elderly found that considerable evidence of the effectiveness and lasting benefits of nondrug treatments for insomnia exist. Compared with the benzodiazepines, the nonbenzodiazepine sedative-hypnotics, such as zopiclone, offer few if any advantages in efficacy or tolerability in elderly persons. Newer agents such as the melatonin receptor agonists may be more suitable and effective for the management of chronic insomnia in elderly people. Long-term use of sedative-hypnotics for insomnia lacks an evidence base and is discouraged for reasons that include concerns about such potential adverse drug effects as cognitive impairment (anterograde amnesia), daytime sedation, motor incoordination, and increased risk of motor vehicle accidents and falls. In addition, the effectiveness and safety of long-term use of nonbenzodiazepine hypnotic drugs remains to be determined.[19]

Reviews
There are no reviews yet.